Dr. Charles Helm (also known as Dr. Dino), with his work featured in a half-dozen Northern Health stories, is well known in Northern BC. He’s an important member of the community of Tumbler Ridge, the town he’s called home for almost 30 years.
For a little over a year, semi-retired Charles has worked with pharmacist Charissa Tonnesen in Tumbler Ridge. Similar teams of doctors, nurse practitioners, and pharmacists collaborated in Chetwynd and Dawson Creek - medical professionals working together to reduce the effects of excessive polypharmacy on Northeastern BC seniors. Polypharmacy means “multiple medications,” and for this project, it was defined as the use of five or more prescribed medications by patients aged 65 years or older. Taking too many medications can lead to unwanted drug interactions, adverse side effects, extra costs, and other problems, particularly as we age and the body processes medications differently.
It’s all about the patients
The aim of the project was that where possible, patients would be able to stop using medications that were no longer necessary. If that wasn’t possible, the teams tried to decrease doses, or aim for once-daily dosing. In rare cases, they prescribed new medications, or increased doses. In Tumbler Ridge, 85 people qualified for this polypharmacy project, and 79 chose to take part. For three-quarters of these patients, the Tumbler Ridge team recommended stopping or reducing medications. For the rest, they recommended increasing doses or starting new medications. In most cases, patients had been on their medications for ten years or more.
“This might be the first time that such a detailed polypharmacy assessment has ever been done on such a high proportion of seniors in a single community,” says Charles.
Charles, Charissa, and their teams reviewed which medications patients were using, what doses they were taking, how long they’d been taking them, and how those medications interacted with each other. “Ultimately it’s about the patients and their quality of life,” says Charles.
Virtual meetings with the health care team
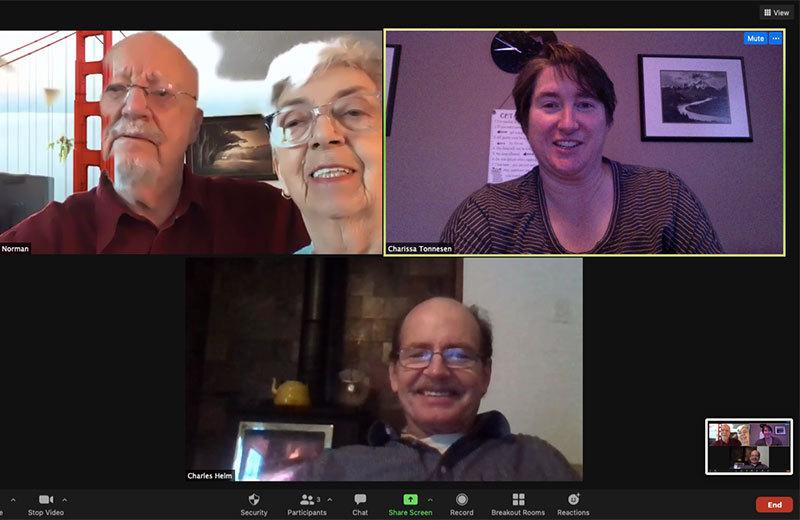
Charles and Charissa also met with each patient and their family members for an hour over Zoom (or on the phone). This team-based approach was the foundation of their project: because both professionals were in the meetings together, they were able to gain a quick, complete understanding of patients’ medical histories and medications. Charles was able to immediately rely on Charissa's pharmacy expertise without having to schedule a separate follow-up appointment to discuss pharmacy research. Likewise, Charissa could also rely in the moment on Charles's medical experience and knowledge.
All of this made it possible for Charles and Charissa to give patients useful suggestions in one appointment, without more follow-up needed between offices. As well, it meant that physician and pharmacist could bounce ideas off of one another. This immediate collaboration often also resulted in unexpected insights that benefitted the patient.
Success stories
While many successes arose from the project, two specific examples stand out to Charles.
The first, he says, illustrates “the gratitude that people felt that we were actually taking an interest in their medications,” – a driving force for him throughout the project. In a story featured by the organization SharedCare, which brings family physicians and specialists together for coordinated patient care, Charles and Charissa discuss a patient in her 70s who had been diagnosed with dementia. As part of the early stages of the polypharmacy project, they assessed her, and after careful consideration, asked her to stop taking a specific drug for pain and anxiety. The medication had worked well in the past, but now seemed to be increasing her confusion. A few weeks after stopping the drug, she was no longer considered to have dementia and was “back to her old self,” to her great relief and that of her family.
In another case, a patient in his 80s had been experiencing ongoing shoulder pain and was unable to lift his arm high enough even to brush his teeth. An operation had not helped. After consultation, Charles and Charissa recommended that he stop a certain medication. Only days later, the patient reported that he was able to brush his teeth again. From there, he progressed to lifting light weights overhead, and is excited to get back into fly fishing.
For Charles, patient empowerment and satisfaction were the most important results of this project. Another key outcome, however, was interprofessional collaboration within the teams. In this project, physicians, pharmacists, nurse practitioners, and other health professionals worked together in their communities. Charles spoke enthusiastically of the value of these partnerships.
Project partnerships
The project was funded by SharedCare, and included the appointment of a project lead, Reina Pharness. Charles speaks highly of both Reina and Charleigh Rudy (Program Specialist working with Divisions of Family Practice), and the skillsets they brought to all of the teams. Their experience and leadership were integral to the success of the project.
Dr. Tom Perry, an internist with the UBC Therapeutics Initiative, also provided specialist support for the project. According to Dr. Perry, this project is a rarity. Collaboration between doctors and other medical health professionals at this level, with this degree of patient follow-up, is not common. At the beginning of this project, meetings with Charles, his team, Reina, and Dr. Perry were exciting, motivating, energetic, and positive. As the project came to a close, meetings were just as encouraging and uplifting as the first time the teams came together.
Excellence in teamwork
“This was probably the single most fulfilling medical work I’ve done,” says Charles. The level of commitment he felt at the beginning did not waver through the project.
“As a total, unexpected spinoff,” says Charles, “I got invited by another pharmacist to send a letter of support for Charissa to nominate her for a BC Pharmacy Award, which I did with pleasure. She won the award and will get it in December. It was really good to see her recognized, not only for her role in our polypharmacy project, but because she’s a great pharmacist.”
Another product of this project was a series of nine webinars for physicians and other health professionals in the region. These educational events were facilitated by the polypharmacy team, and involved discussion of real cases from the region, with attendance varying from 20 to 40 people.
Ultimately, the polypharmacy project aimed to improve patients’ quality of life, reducing drug interactions and side effects and helping keep our elders healthy. The project also brought a team of medical professionals together to try to establish and streamline a new level of care. This collaboration was key for this team, and this experience will be beneficial as they continue to navigate their careers.
To see all completed and ongoing physician quality improvement (PQI) projects across the North, visit the PQI project map.













Comments